Health
Landmark Study Advocates for Newborn Screening for SMA in UK
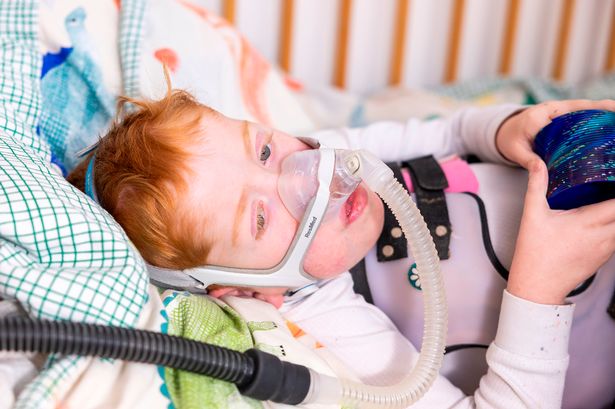
A recent study published in The Lancet emphasizes the urgent need for screening newborns for spinal muscular atrophy (SMA) in the UK, a measure that could save lives and reduce healthcare costs. The findings reveal that the current practice of not including SMA in the NHS newborn heel prick test has led to significant negative outcomes for affected infants.
Since 2019, when the first treatment for SMA became available on the NHS, a total of 507 babies born in the UK have been diagnosed with the condition. Unfortunately, the lack of early screening has resulted in a delayed diagnosis, with the average age for the most severe Type 1 SMA being just six months. This delay has dire consequences; none of the 188 babies diagnosed with this severe form have developed the ability to walk, and many require breathing support or feeding tubes. Tragically, 16 infants diagnosed with SMA have died since 2019.
The study compared the situation in the UK with that in southern Belgium, where newborn screening for SMA is standard practice. In Belgium, all diagnosed SMA babies have survived, and they have achieved significant developmental milestones thanks to immediate treatment after birth. This stark contrast highlights the critical importance of early intervention.
The research, led by Professor Laurent Servais, underscores that the UK’s decision in 2018 to exclude SMA from newborn screening—despite overwhelming support from the SMA community and international evidence—has resulted in poorer health outcomes for children. The paper states, “The 2018 decision… resulted in substantially different outcomes for children born in the UK compared with those born in many other countries where newborn screening is available.”
Cost analysis further illustrates the financial implications of this oversight. Supporting an SMA baby in the UK can cost approximately £74,000 annually, significantly higher than the £25,000 estimated for those identified through newborn screening. These figures reveal not only the personal toll on families but also the financial burden on the NHS.
Despite these findings, the UK National Screening Committee has opted for additional research rather than immediate implementation of a nationwide screening program. A pilot program in select areas of England is in the works, but a full rollout is not anticipated before 2031. In contrast, NHS Scotland has announced plans to include SMA screening in their routine heel prick test starting in spring 2024.
The campaign for SMA screening has gained momentum, particularly from media outlets like The Mirror, which has highlighted individual cases, such as that of Ezra Thorman, a nine-year-old boy with Type 1 SMA who was diagnosed late. His story exemplifies the urgent need for systematic screening to prevent unnecessary suffering.
SMA affects the SMN1 gene, essential for producing a protein that maintains the health of nerve cells responsible for muscle movement. Without this protein, motor neurons degenerate, leading to muscle weakness and atrophy. Fortunately, there are now three treatments approved by the NHS that can significantly alter the disease’s progression, including Zolgensma, a gene therapy that delivers a healthy copy of the SMN1 gene.
Professor Servais has called for immediate action, stating, “SMA is a disease which patients get weaker and weaker by day. It’s a terrible condition but it’s a condition for which we have treatments. From an ethical, medical, clinical, and economic point of view, screening is just a no-brainer.”
The Department of Health and Social Care has acknowledged the importance of ongoing research in this area. A spokesperson indicated, “We welcome research that helps inform our approach to screening. The UK National Screening Committee has recommended a large-scale study into newborn screening for SMA. Hundreds of thousands of babies will be screened for SMA.”
As the debate continues, the evidence mounts in favor of integrating SMA screening into the NHS newborn blood spot test. The potential to save lives and reduce long-term healthcare costs makes a compelling case for change.
-

 World4 months ago
World4 months agoCoronation Street’s Shocking Murder Twist Reveals Family Secrets
-

 Entertainment4 months ago
Entertainment4 months agoAndrew Pierce Confirms Departure from ITV’s Good Morning Britain
-

 Health7 months ago
Health7 months agoKatie Price Faces New Health Concerns After Cancer Symptoms Resurface
-

 Health3 months ago
Health3 months agoSue Radford Reveals Weight Loss Journey, Shedding 12–13 kg
-

 Entertainment8 months ago
Entertainment8 months agoKate Garraway Sells £2 Million Home Amid Financial Struggles
-
 Entertainment4 weeks ago
Entertainment4 weeks agoJordan Brook Faces Health Crisis in Hospital as Sophie Kasaei Stays Away
-

 World5 months ago
World5 months agoEastEnders’ Nicola Mitchell Faces Unexpected Pregnancy Crisis
-

 World5 months ago
World5 months agoBailey Announces Heartbreaking Split from Rebecca After Reunion
-

 Entertainment7 months ago
Entertainment7 months agoAnn Ming Reflects on ITV’s ‘I Fought the Law’ Drama
-

 Entertainment2 months ago
Entertainment2 months agoSelena Gomez’s Name Linked to Epstein: Examining the Claims
-

 Health7 months ago
Health7 months agoTOWIE Stars Sophie Kasaei and Jordan Brook Pursue Fertility Treatment
-

 Health8 months ago
Health8 months agoFiona Phillips’ Husband Shares Heartbreaking Update on Her Health





















